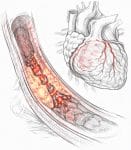
Atherosclerosis is the foundational pathological process underlying the majority of coronary artery disease, ischemic stroke, peripheral arterial disease, and related cardiovascular conditions that collectively represent the leading cause of death and disability worldwide. Far from being a simple plumbing problem of cholesterol-clogged arteries, as the condition is frequently depicted in lay descriptions, atherosclerosis is an extraordinarily complex, decades-long inflammatory disease of the arterial wall in which lipid accumulation, immune cell infiltration, smooth muscle cell migration, extracellular matrix deposition, and progressive structural remodeling of the vessel wall produce the focal plaques whose rupture and subsequent thrombosis are responsible for the acute myocardial infarctions and strokes that kill millions of people annually. The central role of elevated blood cholesterol, particularly low-density lipoprotein cholesterol, in initiating and sustaining the atherosclerotic process has been established by a century of converging evidence from human genetic studies, epidemiological research, animal experiments, and randomized clinical trials, making hypercholesterolemia the most thoroughly validated causal risk factor for cardiovascular disease and the most important single pharmacological target in cardiovascular prevention.
The global burden of atherosclerotic cardiovascular disease is staggering in its magnitude and in its unequal distribution across populations and geographic regions. Coronary artery disease alone causes approximately nine million deaths annually worldwide, making it the single leading cause of death in most countries and accounting for more years of life lost to premature death than any other condition. The economic costs of atherosclerotic cardiovascular disease, encompassing acute hospital care for myocardial infarction and stroke, long-term medications for secondary prevention, cardiac rehabilitation, and the productivity losses from premature death and disability, represent the largest single component of healthcare expenditure in most developed economies. The global convergence of cardiovascular risk factor prevalence, as the epidemiological transition of industrializing nations brings Western dietary patterns, sedentary lifestyles, and growing rates of obesity, diabetes, and hypertension to populations previously protected by traditional diets and physically active lifestyles, means that atherosclerotic cardiovascular disease is rapidly becoming an equally devastating burden in low-income and middle-income countries that previously bore predominantly infectious disease mortality.
The understanding of how elevated cholesterol causes atherosclerosis has been progressively refined over the past century from the early observations of Nikolai Anichkov demonstrating that dietary cholesterol feeding produced aortic atherosclerosis in rabbits, through the landmark Framingham Heart Study epidemiological findings establishing the continuous, graded relationship between serum cholesterol and cardiovascular risk in humans, to the genomic era insights from Mendelian randomization studies demonstrating causality beyond association and from the clinical trials of increasingly potent cholesterol-lowering therapies that have provided the most compelling interventional evidence for the causal role of elevated low-density lipoprotein cholesterol in atherosclerotic cardiovascular disease.
Cholesterol Metabolism and Lipoprotein Biology
Cholesterol is an essential structural component of all mammalian cell membranes, a precursor for the biosynthesis of steroid hormones, bile acids, and vitamin D, and a critical component of the lipid rafts that organize membrane protein function and intracellular signaling. Because of its hydrophobic nature and insolubility in the aqueous environment of plasma, cholesterol is transported in the circulation as a cargo of lipoprotein particles, spherical assemblages of lipid and protein whose surface coat of phospholipids and apolipoproteins renders the hydrophobic core of cholesterol esters and triglycerides compatible with the aqueous circulation. The different lipoprotein classes, distinguished by their density, size, lipid composition, and apolipoprotein content, serve distinct physiological functions and have profoundly different relationships with atherosclerotic risk.
Low-density lipoprotein, produced as the endpoint of the metabolism of very-low-density lipoprotein triglyceride-rich particles secreted by the liver, is the primary transporter of cholesterol from the liver to peripheral tissues and is the lipoprotein class most directly implicated in atherosclerosis pathogenesis. The atherogenicity of low-density lipoprotein particles reflects their small size, which allows them to traverse the endothelial barrier and penetrate into the subendothelial space of the arterial intima, their retention in the subendothelial matrix through ionic interactions between their apolipoprotein B-100 component and proteoglycans of the extracellular matrix, and their susceptibility to oxidative and enzymatic modification in the inflammatory environment of the subendothelial space, generating the oxidatively modified low-density lipoprotein that is the primary driver of macrophage foam cell formation and inflammatory amplification in the developing atherosclerotic plaque.
The low-density lipoprotein receptor, expressed on hepatocyte surfaces and responsible for the receptor-mediated endocytosis of low-density lipoprotein particles that clears them from the circulation, is the key determinant of plasma low-density lipoprotein cholesterol concentration. The molecular regulation of low-density lipoprotein receptor expression, governed by the sterol regulatory element-binding protein pathway that increases receptor expression when intracellular cholesterol levels are low and decreases it when cholesterol is abundant, explains the compensatory response of the liver to dietary cholesterol intake and the mechanisms by which both dietary modification and pharmacological interventions influence plasma low-density lipoprotein cholesterol levels. The proprotein convertase subtilisin-kexin type 9 protein, which promotes the degradation of low-density lipoprotein receptors following their endocytosis, has emerged as a major regulatory target for therapeutic cholesterol lowering following the discovery that loss-of-function mutations in PCSK9 produce very low plasma low-density lipoprotein cholesterol levels with a corresponding dramatic reduction in cardiovascular event risk.
High-density lipoprotein, synthesized in the liver and intestine and receiving cholesterol from peripheral tissues through the process of reverse cholesterol transport, has long been considered cardioprotective based on the strong inverse epidemiological association between high-density lipoprotein cholesterol levels and cardiovascular event risk observed in multiple large population studies. However, the failure of multiple pharmacological strategies that raise high-density lipoprotein cholesterol, including niacin and cholesteryl ester transfer protein inhibitors, to reduce cardiovascular events in randomized clinical trials has substantially complicated the interpretation of high-density lipoprotein cholesterol as a causal protective factor, suggesting that the epidemiological association may reflect the high-density lipoprotein particle functioning as a marker of overall lipid metabolism health rather than itself being the causally protective entity. The focus in contemporary cardiovascular risk reduction has therefore shifted toward the reduction of atherogenic apolipoprotein B-containing lipoproteins as the primary therapeutic target.
The Atherosclerotic Plaque: Formation and Progression
The initiation of atherosclerosis begins at sites of altered endothelial shear stress, particularly at arterial branch points, curvatures, and bifurcations where turbulent and oscillatory flow patterns disrupt the atheroprotective laminar shear stress environment that maintains endothelial cell quiescence, anti-inflammatory gene expression, and nitric oxide production. At these predilection sites, the endothelium transitions to an activated pro-inflammatory phenotype characterized by upregulation of adhesion molecules including vascular cell adhesion molecule-1 and intercellular adhesion molecule-1 that recruit circulating monocytes to the vessel wall, increased endothelial permeability that allows the passage of low-density lipoprotein particles into the subendothelial space, and reduced nitric oxide bioavailability from the uncoupling of endothelial nitric oxide synthase by oxidative stress.
Low-density lipoprotein particles retained in the subendothelial space undergo progressive oxidative modification by the reactive oxygen species generated by activated endothelial cells, infiltrating macrophages, and smooth muscle cells, converting native low-density lipoprotein into oxidized low-density lipoprotein species that are recognized by scavenger receptors on macrophages. Macrophages derived from monocytes recruited to the subendothelial space ingest oxidized low-density lipoprotein through their scavenger receptors in a process that is not subject to the normal cholesterol-dependent downregulation of receptor expression that controls low-density lipoprotein receptor-mediated uptake, allowing macrophages to continue ingesting lipid until they are engorged with cholesterol esters and transformed into the lipid-laden foam cells that are the pathological hallmark of early atherosclerosis. The accumulation of foam cells in the subendothelial space produces the earliest visible atherosclerotic lesion, the fatty streak, which is detectable in coronary arteries of young adults and even children in populations with high-fat dietary patterns.
The progression from fatty streak to clinically significant fibrous plaque involves the migration and proliferation of arterial smooth muscle cells from the medial layer into the intima, where they produce collagen, elastin, and proteoglycans that form the fibrous cap overlying the lipid-rich necrotic core of the mature atherosclerotic plaque. The necrotic core, containing free cholesterol from the membrane lipids of dead foam cells, extracellular lipid droplets, cellular debris, and the remnants of cholesterol crystals that form as cholesterol concentrations in the core exceed its solubility limits, is the most thrombogenic component of the mature plaque and is the material exposed to the bloodstream when plaque rupture or erosion triggers the acute thrombotic events causing myocardial infarction and stroke. The vulnerability of a plaque to rupture is determined by the balance between the mechanical strength of its fibrous cap and the shear forces exerted on it by flowing blood, with plaques characterized by large necrotic cores, thin fibrous caps, and abundant inflammatory infiltrates in the shoulder regions where cap thickness is least being most susceptible to the rupture that precipitates acute cardiovascular events.
Clinical Evidence and Therapeutic Implications
The causal relationship between elevated low-density lipoprotein cholesterol and cardiovascular disease has been validated by multiple lines of evidence that collectively provide one of the most robust causal inference frameworks in clinical medicine. Familial hypercholesterolemia, the genetic disorder producing markedly elevated low-density lipoprotein cholesterol from birth due to mutations in the low-density lipoprotein receptor, APOB, or PCSK9 genes, produces dramatically premature coronary artery disease with myocardial infarctions occurring in the third and fourth decades of life in untreated heterozygotes and in childhood or early adulthood in untreated homozygotes, demonstrating that lifelong low-density lipoprotein cholesterol elevation is sufficient to cause severe atherosclerosis in the absence of other risk factors. Conversely, individuals with loss-of-function mutations in PCSK9 or APOB that produce lifelong very low low-density lipoprotein cholesterol levels show dramatically reduced lifetime cardiovascular event rates, providing the human genetic equivalent of a randomized clinical trial.
The statin class of medications, which inhibit HMG-CoA reductase, the rate-limiting enzyme in cholesterol biosynthesis, and thereby reduce hepatic cholesterol synthesis, upregulate low-density lipoprotein receptor expression, and reduce plasma low-density lipoprotein cholesterol by thirty to sixty percent, have been evaluated in randomized clinical trials involving hundreds of thousands of participants and have consistently demonstrated reductions in major adverse cardiovascular events proportional to the degree of low-density lipoprotein cholesterol lowering achieved. The meta-analyses of statin trials from the Cholesterol Treatment Trialists collaboration, pooling individual patient data from more than 170,000 participants across twenty-seven major trials, demonstrated that each one millimole per liter reduction in low-density lipoprotein cholesterol produces a twenty-two percent reduction in major vascular events including myocardial infarction, coronary death, and stroke, a relationship that is consistent across all risk groups studied and that supports the principle that lower is better for low-density lipoprotein cholesterol in cardiovascular prevention. The extension of cholesterol lowering beyond statins with ezetimibe and PCSK9 inhibitor antibodies including evolocumab and alirocumab has produced further proportional cardiovascular event reductions at very low achieved low-density lipoprotein cholesterol levels, confirming that the benefit-risk balance of extreme low-density lipoprotein cholesterol lowering is favorable in high-risk patients.